Abstract
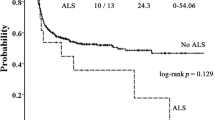
Peri-engraftment respiratory distress syndrome (PERDS) is a kind of potentially life-threatening complication of autologous stem cell transplantation (ASCT). PERDS is characterized by fever, dyspnea, and hypoxemia during neutrophil engraftment. In order to identify the high-risk factors for PERDS, we retrospectively analyzed 260 patients with lymphoma undergoing ASCT in recent five years. The conditioning regimen was BuCyE (busulfan, cyclophosphamide, and etoposide). There were 16 patients (6.1%) diagnosed as PERDS. In multivariate analysis, prior anti-programmed death-1 (PD-1) therapy (hazard ratio [HR] = 8.852, 95% confidence interval [CI]: 2.954–26.527, P < 0.001) and history of pulmonary disease (HR = 3.718, 95% CI: 1.197–11.545, P = 0.023) were independent risk factors for PERDS. Patients with prior anti-PD-1 therapy (n = 31) had higher incidence of engraftment syndrome (77.4% vs. 33.4%, P < 0.001), PERDS (25.8% vs. 3.5%, P < 0.001), and transplant-related mortality (9.7% vs. 0.4%, P < 0.001), compared with those without prior anti-PD-1 therapy (n = 229). Subgroup analysis showed that sintilimab seemed to be associated with higher incidence of PERDS (42.9% vs. 11.8%, P = 0.06) compared with non-sintilimab group (pembrolizumab or toripalimab). C-reactive protein might be a feasible early predictor for PERDS. In conclusion, our study suggests that prior anti-PD-1 therapy may be a strong risk factor for life-threatening PERDS in patients with lymphoma undergoing ASCT.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Spitzer TR. Engraftment syndrome following hematopoietic stem cell transplantation. Bone Marrow Transplant. 2001;27:893–8.
Maiolino A, Biasoli I, Lima J, Portugal AC, Pulcheri W, Nucci M. Engraftment syndrome following autologous hematopoietic stem cell transplantation: definition of diagnostic criteria. Bone Marrow Transplant. 2003;31:393–7.
Cornell RF, Hari P, Drobyski WR. Engraftment syndrome after autologous stem cell transplantation: an update unifying the definition and management approach. Biol Blood Marrow Transplant. 2015;21:2061–8.
Capizzi SA, Kumar S, Huneke NE, Gertz MA, Inwards DJ, Litzow MR, et al. Peri-engraftment respiratory distress syndrome during autologous hematopoietic stem cell transplantation. Bone Marrow Transplant. 2001;27:1299–303.
Yadav H, Nolan ME, Bohman JK, Cartin-Ceba R, Peters SG, Hogan WJ, et al. Epidemiology of acute respiratory distress syndrome following hematopoietic stem cell transplantation. Crit Care Med. 2016;44:1082–90.
Lee CK, Gingrich RD, Hohl RJ, Ajram KA. Engraftment syndrome in autologous bone marrow and peripheral stem cell transplantation. Bone Marrow Transplant. 1995;16:175–82.
Kawano C, Muroi K, Kuribara R, Matsumoto Y, Ohtsuki T, Hatake K, et al. Engraftment syndrome after autologous peripheral blood stem cell transplantation with high numbers of peripheral blood stem cells followed by granulocyte colony-stimulating factor administration. Bone Marrow Transplant. 2000;25:228–9.
Oyama Y, Cohen B, Traynor A, Brush M, Rodriguez J, Burt RK. Engraftment syndrome: a common cause for rash and fever following autologous hematopoietic stem cell transplantation for multiple sclerosis. Bone Marrow Transplant. 2002;29:81–5.
Gonzalez-Vicent M, Ramirez M, Sevilla J, Perez A, Fernandez S, Madero L, et al. Engraftment syndrome after autologous peripheral blood progenitor cell transplantation in pediatric patients: a prospective evaluation of risk factors and outcome. Bone Marrow Transplant. 2004;34:1051–5.
Kanda J, Kaynar L, Kanda Y, Prasad VK, Parikh SH, Lan L, et al. Pre-engraftment syndrome after myeloablative dual umbilical cord blood transplantation: risk factors and response to treatment. Bone Marrow Transplant. 2013;48:926–31.
Xu C, Chen YP, Du XJ, Liu JQ, Huang CL, Chen L, et al. Comparative safety of immune checkpoint inhibitors in cancer: systematic review and network meta-analysis. BMJ. 2018;363:k4226.
Tone M, Izumo T, Awano N, Kuse N, Inomata M, Jo T, et al. High mortality and poor treatment efficacy of immune checkpoint inhibitors in patients with severe grade checkpoint inhibitor pneumonitis in non-small cell lung cancer. Thorac Cancer. 2019;10:2006–12.
Wang H, Guo X, Zhou J, Li Y, Duan L, Si X, et al. Clinical diagnosis and treatment of immune checkpoint inhibitor-associated pneumonitis. Thorac Cancer. 2020;11:191–7.
Knoll BM, Ahmed J, Karass M, Aujla A, McHale P, Kretschmer P, et al. Procalcitonin as a biomarker to differentiate bacterial infections from engraftment syndrome following autologous hematopoietic stem cell transplantation for multiple myeloma. Am J Hematol. 2019;94:E74–6.
Ravoet C, Feremans W, Husson B, Majois F, Kentos A, Lambermont M, et al. Clinical evidence for an engraftment syndrome associated with early and steep neutrophil recovery after autologous blood stem cell transplantation. Bone Marrow Transplant. 1996;18:943–7.
Konuma T, Kohara C, Watanabe E, Mizukami M, Nagai E, Oiwa-Monna M, et al. Cytokine profiles of pre-engraftment syndrome after single-unit cord blood transplantation for adult patients. Biol Blood Marrow Transplant. 2017;23:1932–8.
Jadus MR, Wepsic HT. The role of cytokines in graft-versus-host reactions and disease. Bone Marrow Transplant. 1992;10:1–14.
Borghaei H, Paz-Ares L, Horn L, Spigel DR, Steins M, Ready NE, et al. Nivolumab versus docetaxel in advanced nonsquamous non-small-cell lung cancer. N. Engl J Med. 2015;373:1627–39.
Brahmer J, Reckamp KL, Baas P, Crino L, Eberhardt WE, Poddubskaya E, et al. Nivolumab versus docetaxel in advanced squamous-cell non-small-cell lung cancer. N. Engl J Med. 2015;373:123–35.
Garon EB, Rizvi NA, Hui R, Leighl N, Balmanoukian AS, Eder JP, et al. Pembrolizumab for the treatment of non-small-cell lung cancer. N. Engl J Med. 2015;372:2018–28.
Rittmeyer A, Barlesi F, Waterkamp D, Park K, Ciardiello F, von Pawel J, et al. Atezolizumab versus docetaxel in patients with previously treated non-small-cell lung cancer (OAK): a phase 3, open-label, multicentre randomised controlled trial. Lancet. 2017;389:255–65.
Cho JY, Kim J, Lee JS, Kim YJ, Kim SH, Lee YJ, et al. Characteristics, incidence, and risk factors of immune checkpoint inhibitor-related pneumonitis in patients with non-small cell lung cancer. Lung Cancer. 2018;125:150–6.
Suresh K, Voong KR, Shankar B, Forde PM, Ettinger DS, Marrone KA, et al. Pneumonitis in non-small cell lung cancer patients receiving immune checkpoint immunotherapy: incidence and risk factors. J Thorac Oncol. 2018;13:1930–9.
Chai QQ, Du JY, Zhu J, Wu B. The differences in the safety and tolerability of immune checkpoint inhibitors as treatment for non-small cell lung cancer and melanoma: network meta-analysis and systematic review. Front Pharmacol. 2019;10:1260.
Acknowledgements
We thank all the patients, their families, and other clinical staff for their participation in the study.This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
H-QH, Q-CC and BB designed the research, collected the data, interpreted the data, and wrote the manuscript; X-XW, YG, P-FL, H-XH, CH and L-QP were involved in treating patients, collecting data, and writing the manuscript. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Bai, B., Wang, XX., Gao, Y. et al. Prior anti-PD-1 therapy as a risk factor for life-threatening peri-engraftment respiratory distress syndrome in patients undergoing autologous stem cell transplantation. Bone Marrow Transplant 56, 1151–1158 (2021). https://doi.org/10.1038/s41409-020-01164-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41409-020-01164-y